Aggregatibacter actinomycetemcomitans (A.a.)
(A.a.) is known for its ability to evade normal immune defenses and produce toxins that can damage gum tissue and bone. It has been strongly associated with localized aggressive gum disease and can persist even in individuals with good oral hygiene. Because A.a. can remain active at low levels and resist routine cleaning alone, identifying its presence is an important step in understanding individual risk and guiding more targeted preventive care.
Why Aggregatibacter actinomycetemcomitans Is Clinically Important
A.a. is distinctive among oral bacteria because it produces virulence factors, including leukotoxin, that can impair the body’s immune cells and weaken local defenses. This allows the organism to persist below the gumline and contribute to bone and tissue breakdown even when brushing and flossing appear adequate. Its ability to survive undetected makes it an important organism to identify when evaluating unexplained inflammation or localized periodontal changes.
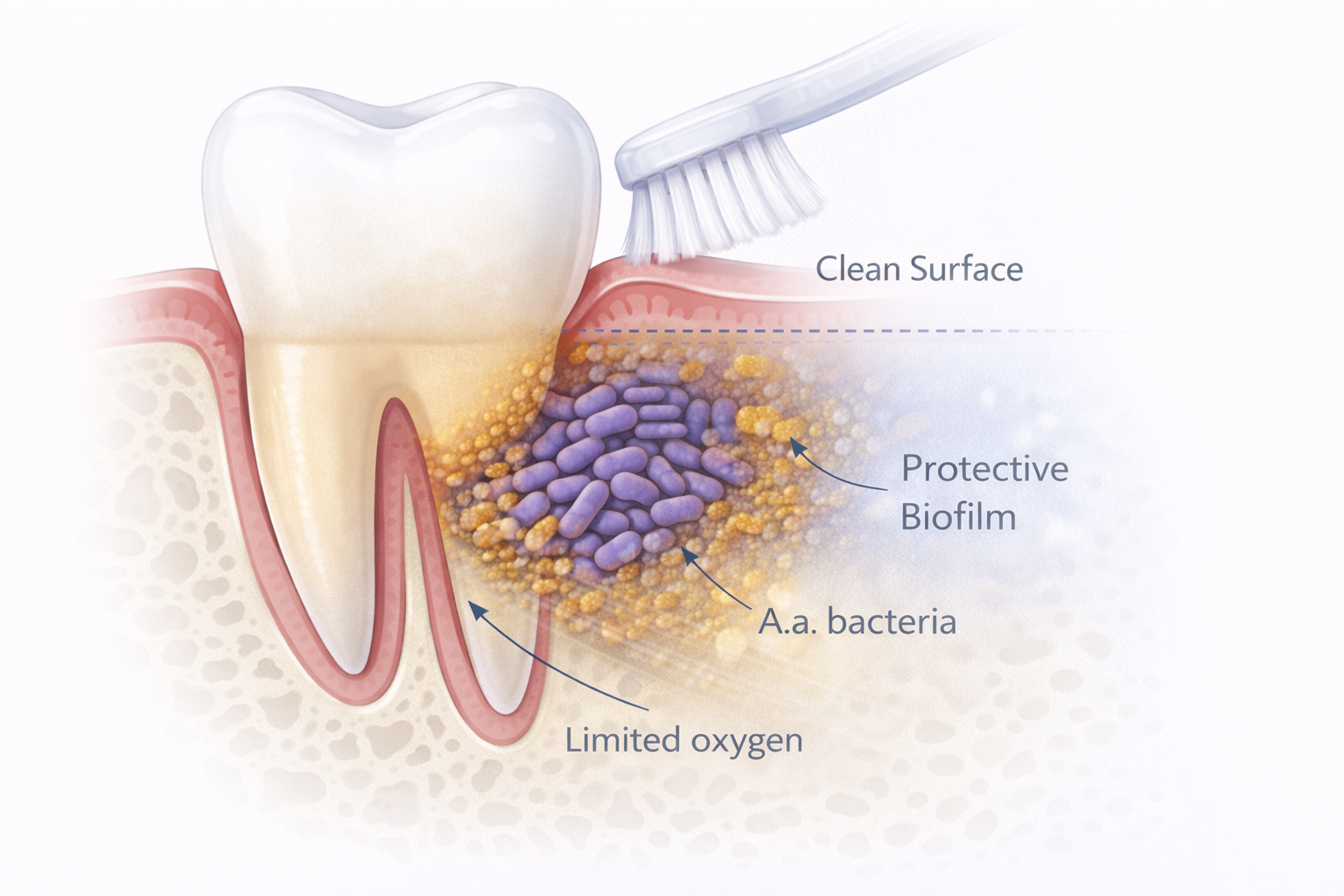
Why A.a. Can Persist Despite Good Oral Hygiene
A.a. is especially adept at surviving in deep periodontal pockets and areas with limited oxygen, where routine brushing and flossing have little effect. It can adhere tightly to tooth and root surfaces and integrate into complex biofilms that protect it from mechanical disruption. As a result, patients may maintain excellent daily oral care yet still harbor this organism below the gumline, highlighting the need for more individualized assessment.
The oral–systemic connection
Research shows that Aggregatibacter actinomycetemcomitans (A.a.) is not confined to the mouth. This bacterium has been linked to increased systemic inflammation and has been associated with elevated risks involving the cardiovascular system, immune system dysregulation, and inflammatory burden throughout the body. Studies have also explored connections between A.a. and conditions such as atherosclerosis, adverse pregnancy outcomes, and inflammatory joint and metabolic processes. Because the gums are highly vascular, harmful bacteria like A.a. can enter the bloodstream—especially when gum tissues are inflamed or the body’s defenses are overwhelmed—allowing oral infections to influence overall health far beyond the teeth and gums.
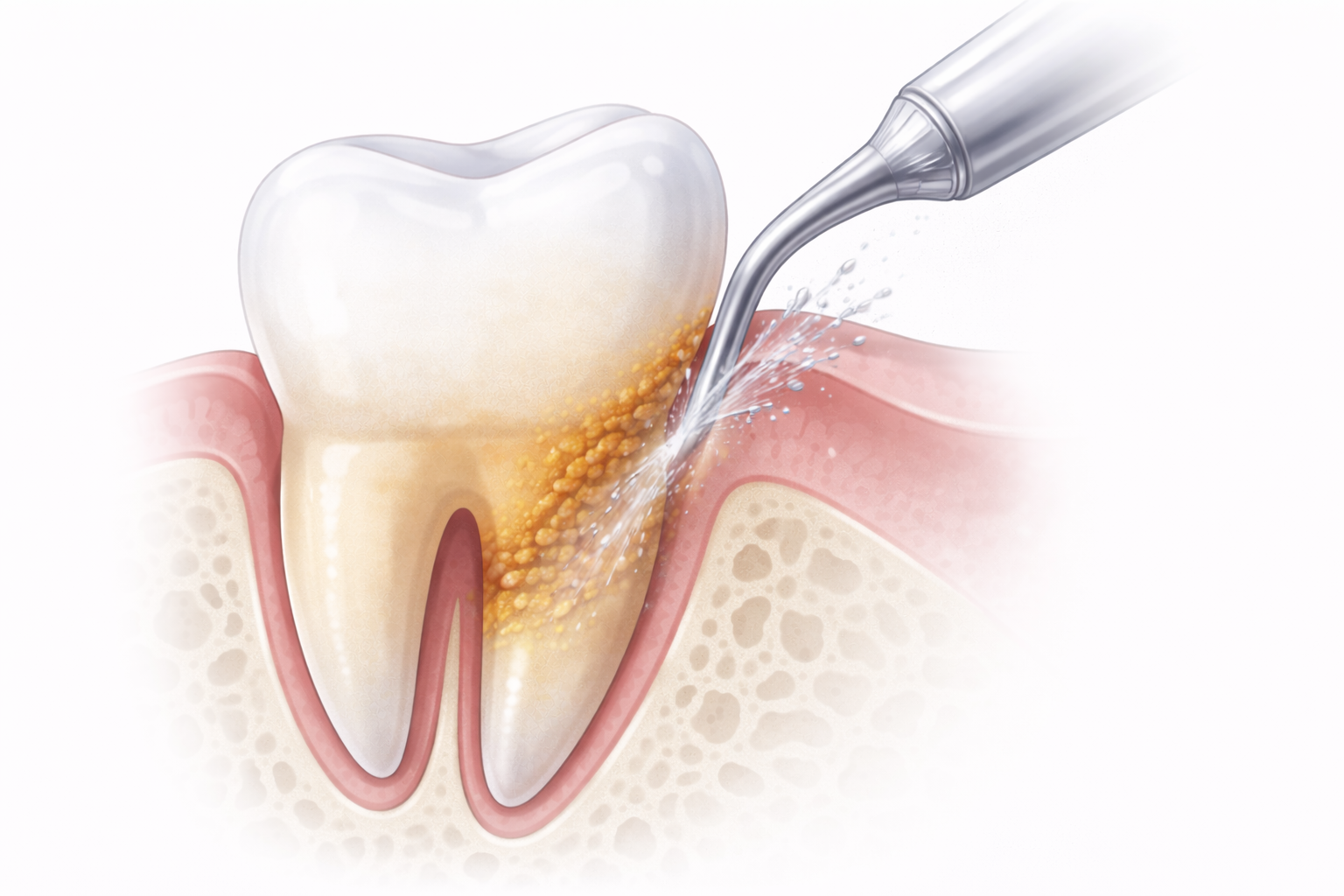
How A.a. is treated
Treating Aggregatibacter actinomycetemcomitans (A.a.) requires a targeted and strategic approach because this bacterium can invade gum tissue and resist routine cleanings alone. Management typically involves professional disruption of pathogenic biofilm, reduction of bacterial load within deep periodontal pockets, and the use of antimicrobial or oxygen-based therapies designed to reach areas brushing and flossing cannot. In many cases, guided at-home treatments are incorporated to maintain control between visits, along with support for a healthier oral microbiome. Ongoing monitoring through salivary diagnostics allows treatment to be adjusted over time, with the goal of long-term bacterial control, preservation of bone, and protection of both oral and systemic health.
FAQs
-
Aggregatibacter actinomycetemcomitans possesses several defense mechanisms that allow it to survive despite the body’s immune response and routine dental care. It produces powerful toxins, including leukotoxin, which impair white blood cells and weaken local immune defenses. A.a. can invade and persist within gum tissue, shielding itself from mechanical cleaning and some antimicrobial agents. It also forms structured biofilms that limit oxygen penetration and reduce treatment effectiveness, while certain strains demonstrate the ability to evade host defenses and adapt to hostile environments. These protective strategies help explain why A.a. can cause significant bone loss with few symptoms and why targeted, ongoing management is often necessary.
-
Yes, Aggregatibacter actinomycetemcomitans (A.a.) can be transmitted between close contacts, including family members. Research suggests that A.a. may spread through saliva-sharing activities such as kissing, sharing utensils, or other close oral contact, which is why it is sometimes found clustering within families. However, transmission alone does not guarantee disease—whether A.a. becomes problematic depends on individual factors such as immune response, oral hygiene, inflammation, and overall health. This is one reason saliva testing and individualized monitoring can be helpful, especially when aggressive periodontal disease appears in multiple family members.
-
Aggregatibacter actinomycetemcomitans (A.a.) is very different from typical plaque bacteria. While most plaque bacteria remain on the tooth surface and mainly contribute to cavities or mild gum inflammation, A.a. is far more aggressive. It can invade gum tissue, evade the immune system, and produce toxins that damage the body’s natural defenses. Unlike common plaque bacteria that are usually controlled with brushing and routine cleanings, A.a. can cause rapid bone loss with few visible symptoms and often requires targeted, ongoing management to keep it under control.
-
No. Having Aggregatibacter actinomycetemcomitans (A.a.) does not automatically mean tooth loss. It means a higher-risk bacterium has been identified, which allows us to be proactive rather than reactive. Many patients with A.a. maintain their teeth long-term with early detection, targeted treatment, and ongoing monitoring. The key is managing the bacteria and controlling inflammation before significant bone loss occurs, which is exactly why saliva testing and personalized care plans are so important.
